Advanced Mechanical Modeling and Simulation Drive Innovations in Lung Ventilation
The complex interplay between airflow and tissue deformation within human lungs is one of the most significant and challenging aspects of respiratory biomechanics. As gas moves through the branching airway tree, the surrounding parenchyma (i.e., the functional lung tissue) undergoes intricate, complex, and heterogeneous deformation. The characterization of such mechanical processes is crucial for the prediction of ventilation heterogeneity, monitoring of lung disease progression, and assessment of the potential for ventilator-induced lung injury (VILI). To better understand such complicated dynamics, our research groups at Morgan State University and the University of Iowa are leveraging anatomically resolved geometries and time-dependent computational fluid dynamics (CFD) to create high-fidelity “digital lung” models. These models allow us to analyze the influence of varying ventilation waveforms on intrapulmonary airflow and the effect of different constitutive descriptions on predicted tissue deformation [1, 6, 7].
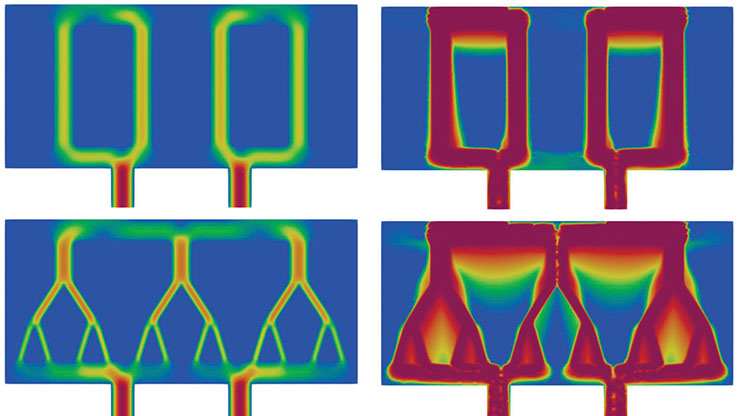
![<strong>Figure 1.</strong>Multifrequency ventilation (MFV) incorporates fast oscillatory components (3.5 and 7 Hertz) to produce rich intra-airway interactions. <strong>1a.</strong> Application of two flow waveforms at the trachea (inlet) for conventional mechanical ventilation (CMV) (top) and MFV (bottom) simulations. <strong>1b.</strong> The velocity profiles under MFV conditions. Figure courtesy of [6], with permission.](/media/0myczg4e/figure1.jpg)
CFD Modeling and Simulation of Airway Ventilation
In respiratory mechanics, the airway pressure at the ventilator inlet—denoted by \(P \) as a function of time \(t\)—is commonly represented via a single compartment-based formulation [2]:
\[P(t) = \frac{V(t)}{C_{rs}} + R_{rs}\dot{V}(t)+P_0. \tag1\]
Here, \(V\) denotes lung volume; \(\dot{V}\) indicates gas flow rate; \(C_{rs}\) and \(R_{rs}\) represent respiratory system compliance and resistance, respectively; and \(P_0\) is the positive end-expiratory pressure.
![<strong>Figure 2.</strong> From computed tomography data to finite element mesh. <strong>2a.</strong> Fine-grained pig lung geometry extracted from the computed tomography scan <strong>2b.</strong> Its coarsened mesh. Figure courtesy of [7], with permission.](/media/i2mlhyql/figure2.jpg)
A recent study simulated airflow in a segmented porcine airway tree that extends from the trachea to the fifth generation, assuming gas flow based on the incompressible Navier-Stokes equation [6]. This work prescribed physiologically motivated, dynamic outlet boundary conditions based on downstream elastance and resistance from \((1)\). The resulting simulations in Figure 1 demonstrate that multifrequency ventilation (MFV)—when compared to conventional mechanical ventilation (CMV)—yields higher shear stress and turbulence kinetic energy, giving rise to asymmetric intrapulmonary flow (pendelluft) near the transitions between inspiration and expiration.
Modeling Lung Tissue: Poroelasticity Versus Hyperelasticity
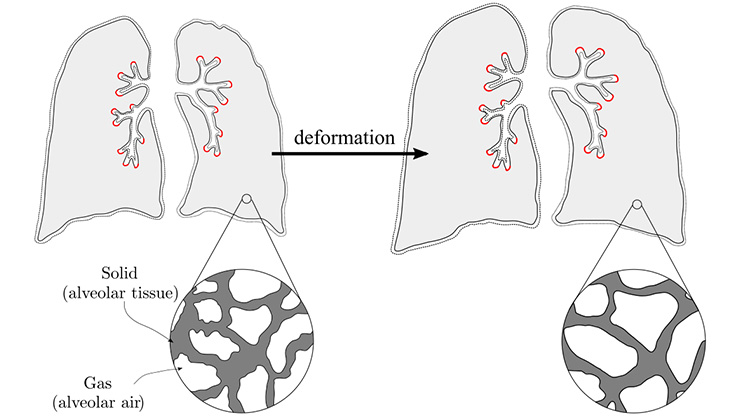
While CFD-based gas flow predicts ventilation distribution under various conditions of lung mechanical heterogeneity, successful models of parenchymal tissue deformation require an appropriate constitutive representation of the tissue. In this context, other recent work [7] used computed-tomography-derived porcine lung geometry and finite element simulations (see Figure 2) to quantitatively compare hyperelastic formulations (Holmes-Mow and neo-Hookean) with a poroelastic model based on the Birzle-Wall framework [3, 4], which accounts for both the solid matrix and air-filled microstructure. Figure 3 depicts conceptual deformation patterns during a single breathing cycle.
![<strong>Figure 3.</strong> Mechanical quantities across the parenchyma geometry at \(t = 2\) seconds according to the poroelastic material values in [8]. Figure courtesy of [7], with permission.](/media/nchpphc0/figure3.jpg)
However, the finite element simulations revealed that hyperelastic models miss key physiologic behaviors [7]. Specifically, the poroelastic formulation predicted a relative volume change \((J\approx 1.20) \) that closely matched experimental volume data \((J_{\textrm{exp}}\approx 1.27),\) whereas both hyperelastic models predicted a much larger expansion \((J\approx 1.43)\) under identical loading. This outcome indicates that poroelasticity is essential to correctly express the interactions between internal tissue pressure, permeability, and deformation — especially during rapidly changing flow rates. By identifying areas of high mechanical strain, we can thus predict potential anatomic sites of further lung injury during mechanical ventilation.
Toward a Physics-based Digital Twin
The integration of gas flow modeling during mechanical ventilation with accurate parenchymal deformation is the foundation for a predictive “digital lung” [5]. Future models must couple airway CFD with poroelastic finite element methods of the parenchyma and realistic boundary conditions to provide real-time guidance for patient-specific risk of VILI. Our collaboration between Morgan State and Iowa has established that MFV produces stronger asymmetric flow and enhanced mixing when compared to CMV. These major steps toward physics-based digital twins have the potential to transform mechanical ventilation strategies and personalize respiratory care for the improved management of acute respiratory distress syndrome and other trauma.
Acknowledgments: Mingchao Cai was supported in part by Army Research Office award W911NF-23-1-0004 and the affiliated project award from the Center for Equitable Artificial Intelligence and Machine Learning Systems at Morgan State University (project ID 02232301). David Kaczka was supported in part by the Office of the Assistant Secretary of Defense for Health Affairs’ Peer Reviewed Medical Research Program under awards W81XWH-16-1-0434 and W81XWH-21-1-0507.
David Kaczka is a co-founder and shareholder of OscillaVent, Inc., and a co-inventor on several patents that involve mechanical ventilation. He also receives research support from ZOLL Medical Corporation and has consultant agreements with Lungpacer Medical, Inc., and Radiatric, Inc. The authors attest that industry had no role in the preparation, review, or approval of the manuscript.
References
[1] Akor, E.A., Han, B., Cai, M., Lin, C.-L., & Kaczka, D.W. (2024). Forward computational modeling of respiratory airflow. Appl. Sci., 14(24), 11591.
[2] Bates, J.H.T. (2009). Lung mechanics: An inverse modeling approach. New York, NY: Cambridge University Press.
[3] Birzle, A.M., Martin, C., Uhlig, S., & Wall, W.A. (2019). A coupled approach for identification of nonlinear and compressible material models for soft tissue based on different experimental setups — exemplified and detailed for lung parenchyma. J. Mech. Behav. Biomed. Mater., 94, 126-143.
[4] Birzle, A.M., Martin, C., Yoshihara, L., Uhlig, S., & Wall, W.A. (2018). Experimental characterization and model identification of the nonlinear compressible material behavior of lung parenchyma. J. Mech. Behav. Biomed. Mater., 77, 754-763.
[5] Gonsard, A., Genet, M., & Drummond, D. (2024). Digital twins for chronic lung diseases. Eur. Respir. Rev., 33(174), 240159.
[6] Han, B., Akor, E.A., Cruz, A.F., Cai, M., & Kaczka, D.W. (2025). Simulation of central airway gas flow dynamics during conventional and multifrequency ventilation. J. Biomech. Eng., 147(10), 101004.
[7] Olabanjo, O., Aigbokhan, E., Akor, E.A., Kaczka, D.W., & Cai, M. (2025). Finite element simulation of lung parenchyma deformation based on porcine data. Comput. Methods Biomech. Biomed. Engin., 1-21.
[8] Shim, J.J., Maas, S.A., Weiss, J.A., & Ateshian, G.A. (2021). Finite element implementation of biphasic-fluid structure interactions in FEBio. J. Biomech. Eng., 143(9), 091005.
About the Authors
Mingchao Cai
Applied mathematician and computational scientist
Mingchao Cai is an applied mathematician and computational scientist with expertise in advanced numerical methods and machine learning and a focus on applications in lung mechanics and biomedical digital twins. He leads interdisciplinary research that integrates mathematical analysis, high-performance computing, and biomechanics to advance translational innovation.
David W. Kaczka
Physician-scientist and biomedical engineer
David W. Kaczka is a physician-scientist and biomedical engineer who contributes to respiratory mechanics, pulmonary imaging, and mechanical ventilation. His work integrates clinical insight with experimental and computational methods to advance overall understanding of lung function, airway dynamics, and the pathophysiology of acute and chronic respiratory diseases.
Related Reading
Stay Up-to-Date with Email Alerts
Sign up for our monthly newsletter and emails about other topics of your choosing.



